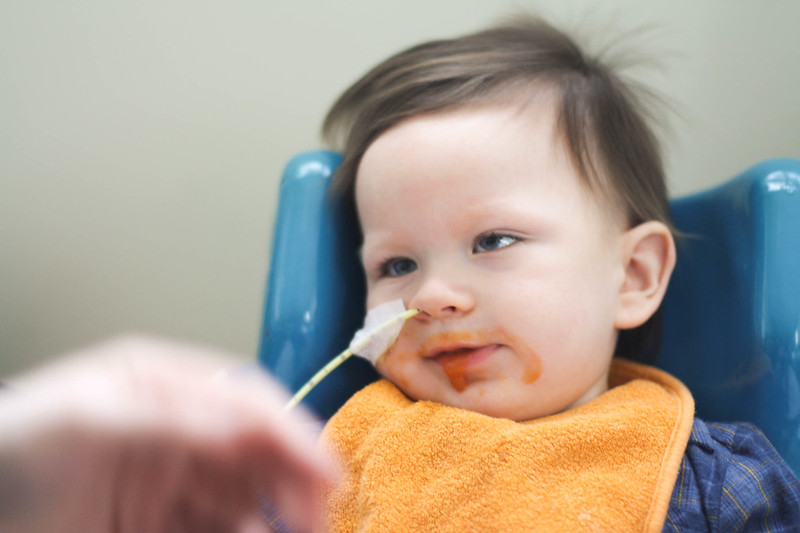
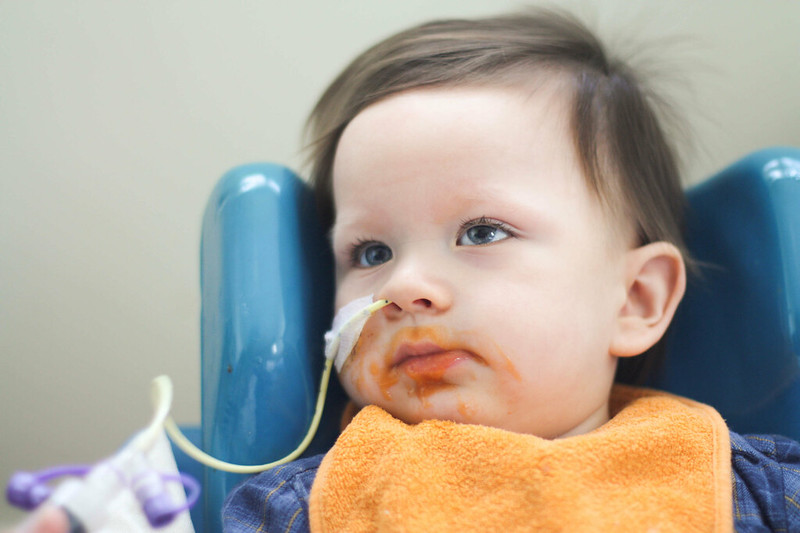
Our speech and language therapist (SALT) came by last week. I like her, she’s lovely. It’s her job to assess Kai’s suck and swallow, ensuring that it’s safe for him to feed. That his swallow is good and his suck solid and that we’re doing everything we can to encourage oral feeding in a manner that’s safe.
She decided that Kai should be nil by mouth. That we should put nothing in his mouth, that his suck was nonexistent (which we knew) and his swallow was unsafe. Kai would hold anything in his mouth in his cheeks. Or not even his cheeks, he’d drool it out if positioned correctly.
100% tube fed.
That was hard to hear. Also, completely impractical for us. Since he’s been ill, Kai has been maybe 98% tube fed. Part of having the ng tube is that we check each and every time we use it to ensure it’s in his stomach and not in his lungs. Every time. Because every cough or vomit could move the tube up his throat, and it could move from his belly to his lungs. If we put something down the tube and it was in his lungs, we could drown him. Nothing like an element of extreme danger when feeding your own child, hey?
But, to check Kai has to have something in his belly to aspirate – for us to draw up the tube to know it’s in the right place. If we don’t get an aspirate, you can’t just put things down the tube – there’s that risk of drowning.
So we do the aspirate dance. We reposition him, lie him on his left side, sit him up, push a small amount of air down the tube. We pull the tube out slightly and push it back down. If we still don’t get an aspirate (which is most of the time) what we would give him something orally till there was enough in his stomach to get an aspirate.
If Kai is nil by mouth, we’d need to pull the tube out and pass a new one. If we still didn’t get an aspirate (which is likely, because there’s probably nothing wrong with the tube), our nurse’s advice is to go into the a&e and get an X-ray.
Uhm.
No. Just no. I am not taking my kid into the a&e and exposing him to all the risks of the other sick children to get an X-ray and mistime all his meds 3-4 times a day because we can’t get an aspirate. It was the most impractical piece of advice I’d ever heard.
What we need is a gastrostomy, because with a gastro you know it’s in the stomach. It’s surgically placed in the stomach and has zero chance of moving with a cough or a vomit.
But we’re still waiting for that.
So, we very very carefully weigh the risks.
It’s the risk of aspirating something into Kai’s lungs by giving him something oral vs the risk of Kai catching something while we wait in the a&e waiting room, and the risk of increased seizures while his medication schedule is all out of whack while we wait on the hospital time.
There are other considerations: the risk of the tube moving into Kai’s lungs is not zero, but it is small. What’s more, if it’s blocking his airway we should be able to tell, in the same way we can tell when he’s working harder to breathe with the increased secretions of a cold. It’s not a 100% reliable method (and we don’t rely on it) but it’s something to think on.
The second is that Kai is recovering from a horrific respiratory virus. His body is exhausted and everything is out of whack. He’s lost some skills (womp) but we’re hoping it’s a transient loss – that he’ll regain those skills. What’s more, Kai had a seizure before our SALT arrived. She saw Kai for maybe half an hour, at a time when he was particularly low. Her view of his Kai’s ability to suck and swallow is based on that snapshot.
However, my perspective is based on hours and hours with Kai. Sure enough, later in the day when Kai was positively perky, he was showing much more interest in swallowing and sucking. The next day was even better, with him managing a dummy with enthusiasm.
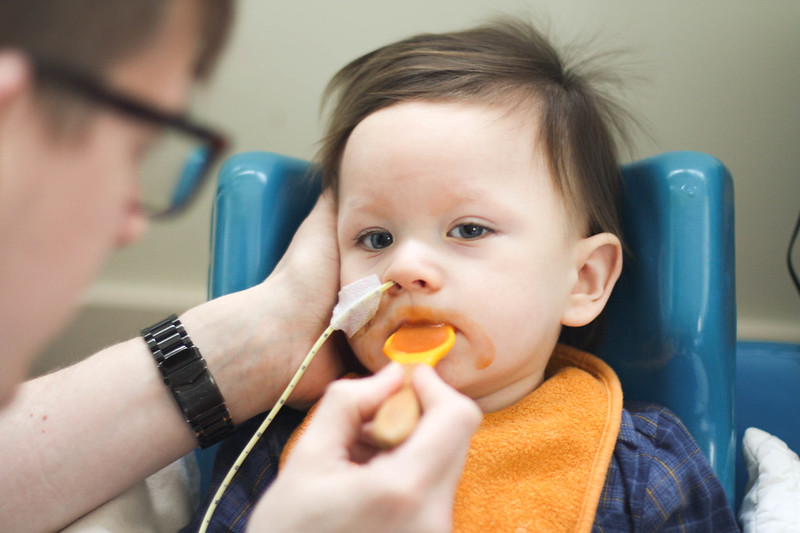
So, I took a calculated risk and fed Kai some purée. Which of course he nommed down like a champ. It wasn’t a lot of purée, maybe an ice cube amount, and it wasn’t pre-illness standards, there was a second swallow to clear what was in his mouth, but he took just enough to enjoy himself and to get an aspirate.
This is one of those moments where I hear what our medical professionals are telling us, and I absolutely consider it, but then I look at Kai and figure out what is really best for him.
If Kai is awake and aware and doing just fine, and managing his secretions, sure, let’s try purée or a bottle. Just a small amount, because I don’t fancy tiring him out eating. But enough to get an aspirate and for him to enjoy the sensation of food in his mouth and for him to use the muscles required for sucking and swallowing.
If Kai was drowsy, or had a seizure earlier in the day or was maybe a bit less with it, I’d never try feed him purée. I might try a tiny amount cooled boiled water if I thought he was awake and aware enough to swallow it (if he aspirated, cooled boiled water is going to be less harmful in his lungs than say a mouthful of chickpea and sun-dried tomato purèe).
If I couldn’t wake him, and he wasn’t managing his secretions I wouldn’t even try the water. I’d take him into a&e for that X-ray.
I’m not an idiot, despite how our medical team dole out advice and insist they know best. My problem is they see Kai for a short amount of time, a tiny snapshot, and make huge sweeping decisions that I’m expected to follow without hesitation or argument. I’m meant to trust our team implicitly.
But they’re just people. Who are sometimes wrong, who don’t look at the big picture and who don’t have the perspective I do. They’re also bound by NHS policy, which is designed for the cost saving average, rather than the wellbeing of Kai specifically.
Becoming a special needs parent is about becoming an expert in your child, and in advocating for Kai, I perhaps stand up to our team more than other parents do. Or at least I get that impression from the manner in which I’m treated when I disagree.
So. I’m feeding my son purée when he’s been declared nil by mouth.
I don’t enjoy being in this position, but hey ho. Bring on that gastrostomy, hey?